Treatment for Peyronie’s disease for men can be done in two ways: injections or surgery. Injections are the more common medical option. The provider will inject lidocaine into the penis to numb it before administering the medications. The bandage should be removed three hours after the injection, but patients should not engage in sexual activity for 24 hours. Steroid injections are most effective in the early stage when Peyronie’s plaque is in its early stages. The medication is injected into the plaque using a fine needle. Local anesthetic agents are not used because they could cause an infection of the vascular corpora.
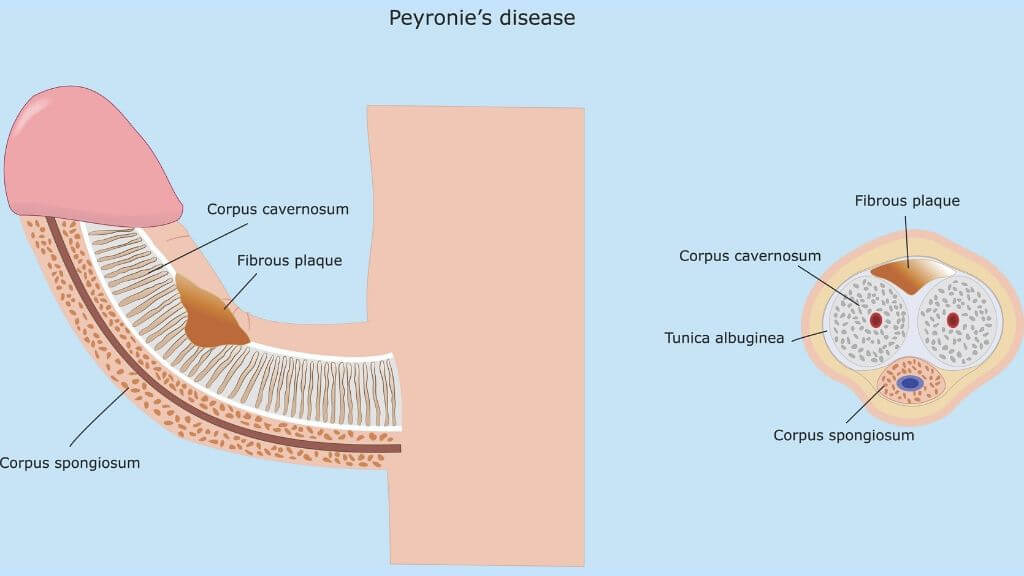
The Men’s Clinic at UCLA is the leader in research and treatment of this condition. Dr. Jesse Mills, who leads the UCLA Peyronie’s disease research, has been the principal investigator for a Phase III clinical trial and a leading expert in the administration of Xiaflex, a prescription medication that treats Peyronie’s. Peyronie’s disease is an abnormal bend in the penis during an erection. Approximately one to five percent of men are affected by Peyronie’s disease.
While Peyronie’s disease can affect any man, its incidence increases with age. Younger men do not usually suffer from the disease, although they may experience a small amount of penile curvature. The disease is not contagious, but certain health conditions are associated with it. Smoking and some types of prostate surgery are linked to Peyronie’s disease in men. So it’s best to visit a doctor if your partner complains about your penile curvature.
If your symptoms do not improve after a few months of self-care, you can visit a physician. They will perform a physical examination and feel for scar tissue. Your doctor may order an ultrasound scan. You may be able to avoid surgery if the curvature is only minor. If you have the disease, your doctor may recommend watchful waiting while the condition worsens. But if your symptoms have become so severe that you cannot engage in sexual activity, it is best to seek medical attention.
In 13 cases out of 100, men who are in the early stage will go away on their own without medical intervention. But it’s important to note that medications for Peyronie’s disease are not FDA-approved. And doctors should only prescribe drugs if they are proven effective for the acute phase of the disease. For men who have milder symptoms, oral treatments are an option. You can also try marketed herbal remedies.
A physical examination can help a health care provider determine if you have Peyronie’s disease. They can also check if the penis is stiff. Sometimes, the health care provider will inject a drug into the penis to make it stiffer. And if you’re concerned, the doctor will take a picture of your penis. Another medical option for diagnosing PD is a dynamic ultrasound. This imaging tool uses sound waves to get a clear picture of where plaques are located. It can also reveal whether there is calcium buildup and blood flow.
Men who are diagnosed with Peyronie’s Disease may be ashamed and feel less manly. They may feel self-conscious about their bent penis, and they may worry that it will turn off a partner. They may be particularly self-conscious if they are gay. There is no single cause of this disease, but many factors contribute to the severity of the symptoms. Regardless of the cause, treatment for Peyronie’s disease can improve your quality of life and reduce your stress levels.
Understanding Peyronie’s disease in men is a good starting point in the treatment process. The condition is a complicated and emotional subject and your partner may feel lost when his penis is absent. Whether you decide to seek treatment or not, talk to someone who has suffered from it. A good sexual medicine expert can recommend reliable books and other materials that will explain the condition in greater detail. If you can’t talk to a specialist, try asking other men in the same situation about their experiences with Peyronie’s disease.
Treatment for Peyronie’s disease in men may be a combination of nonsurgical treatment and medications. Non-surgical treatment is generally recommended for the first 12 months and may be avoided for men with small plaques. Drug therapy is another option for men with acute symptoms, though most guidelines don’t recommend oral drugs or surgery. In severe cases, surgery may be recommended. However, treatment for Peyronie’s disease in men is different for every man.
Medical treatment for Peyronie’s disease in men may include using collagenase (a protein found in human blood), verapamil, and penile traction devices. The latter may be more effective than medical therapy alone. Medical therapy is important for men with Peyronie’s disease, as it improves quality of life. Surgery can also be considered when treating ED with medical therapy has failed to improve erectile function.
Treatment for Peyronie’s disease in men usually begins with a physical exam. A healthcare provider may use a test called ultrasound to check for plaques and check the blood flow. These tests may also reveal the symptoms of the disease, such as a bent/curved penis, and a reduced ability to achieve an erection. In the acute phase of the condition, the penis may lose half of its original length. This is because the penile’s thick fibers lose their elasticity. As the disease progresses, the penis may become smaller.
Treatment for Peyronie’s disease in men includes a collagenase treatment, which is the only FDA-approved medication for Peyronie’s. The treatment also involves avoiding pelvic trauma, which may result in Peyronie’s. While there are no preventive measures for Peyronie’s disease in men, preventing it can help reduce the severity of symptoms and prevent it from recurring.
The cause of Peyronie’s disease in men is unknown, but genetics and environment play a role. Men who have connective tissue disorders are more susceptible. Diabetes and tobacco use are also risk factors. In the majority of cases, Peyronie’s Disease is not painful and can resolve itself on its own within a year. The plaque can become tough fibrous tissue, and calcium deposits may form, but the condition is not cancerous.